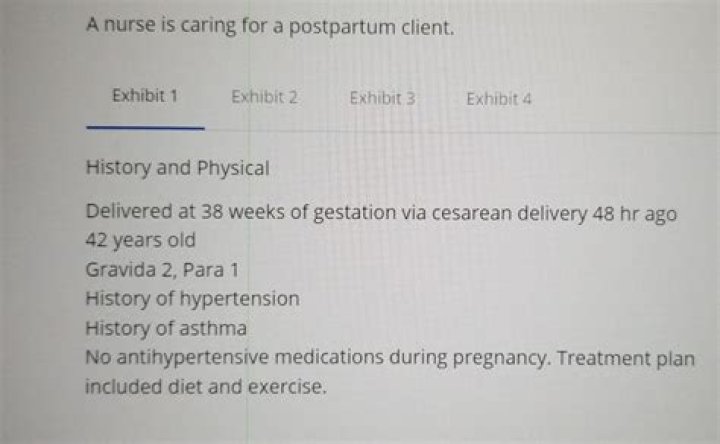
What should the nurse include in the past history of the patient
 Emma Terry
Emma Terry The past health history should elicit information about the patient’s childhood illnesses and immunizations, accidents or traumatic injuries, hospitalizations, surgeries, psychiatric or mental illnesses, allergies, and chronic illnesses.
What information must be included in the health history of a patient?
A personal medical history may include information about allergies, illnesses, surgeries, immunizations, and results of physical exams and tests. It may also include information about medicines taken and health habits, such as diet and exercise.
Which of the following is included in a past medical history?
In general, a medical history includes an inquiry into the patient’s medical history, past surgical history, family medical history, social history, allergies, and medications the patient is taking or may have recently stopped taking.
What should the nurse document in the history component of the health assessment?
A patient states that the pain medication is “not working” and rates his postoperative pain at a 10 on a 1-to-10 scale. Which of these assessment findings indicates an acute pain response to poorly controlled pain? The nurse is preparing to perform a physical assessment.Under which section in the health history will the nurse include?
Under which section in the health history will the nurse include the patient’s name and primary language? While recording the patient’s complete health history, the nurse will record the patient’s personal details such as occupation, ethnicity, and health practices under the biographic data section.
How do nurses take health history?
- General suggestions.
- Elicit current concerns.
- Ask questions.
- Discuss medications with your older patients.
- Gather information by asking about family history.
- Ask about functional status.
- Consider a patient’s life and social history.
What is a nursing health history?
The health history provides nurses with in-depth information about symptoms, childhood illnesses, related medical experiences and risks for developing certain diseases. After the health history data is recorded, a physical is conducted which covers a review of the patient’s body systems.
What is a health history in nursing assessment?
The health history provides nurses with in-depth information about symptoms, childhood illnesses, related medical experiences and risks for developing certain diseases. After the health history data is recorded, a physical is conducted which covers a review of the patient’s body systems.What 10 components should be included in a health history questionnaire?
- Personal status.
- Family and social relationships.
- Diet and Nutrition.
- Functional ability.
- Mental Health.
- Personal Habits.
- Health promotion activities.
- Environment.
- present complaint and nature of symptoms.
- onset of symptoms.
- severity of symptoms.
- classifying symptoms as acute or chronic.
- health history.
- family history.
- social history.
- current medical and/or nursing management.
What should I ask about past medical history?
- Past Medical History: Start by asking the patient if they have any medical problems. …
- Past Surgical History: Were they ever operated on, even as a child? …
- Medications: Do they take any prescription medicines? …
- Allergies/Reactions: Have they experienced any adverse reactions to medications?
How do you write past medical history?
- Step 1: Include the important details of your current problem. Timing – When did your problem start? …
- Step 2: Share your past medical history. List all your past medical problems and surgeries. …
- Step 3: Include your social history. …
- Step 4: Write out your questions and expectations.
What are the 6 components of the medical history?
- Source & Reliability.
- Chief Complaint (CC)
- History of Present Illness (HPI)
- Past Medical History (PMH)
- Social History (SH)
- Family History (FH)
- Review of Systems (ROS)
What data do nurses document under the category of past health history?
Past health history includes the patient’s past illnesses such as childhood illnesses, accidents, hospitalizations, and operations. Because the patient is describing a past accident, it should be documented under the past health history section.
Which factors should the nurse incorporate into the assessment of an older client according to the acronym spices select all that apply?
SPICES is an acronym for a brief protocol for multidimensional assessment to identify risk factors related to caring for older adults: skin integrity; problems eating; incontinence; confusion; evidence of falls; and sleep disturbance [4].
What is a detailed assessment of a patient's medical history?
A medical chart is a complete record of a patient’s key clinical data and medical history, such as demographics, vital signs, diagnoses, medications, treatment plans, progress notes, problems, immunization dates, allergies, radiology images, and laboratory and test results.
What are the 7 parts of the health history?
- ID. Identifying data, source of hx, reliability.
- CC. Chief concern.
- PI. Present illness.
- PH. Past history.
- FH. Family History.
- P/S H. Persona/Social History.
- ROS. Review of Systems.
What are the 4 types of nursing assessments?
In order to effectively determine a diagnosis and treatment for a patient, nurses make four assessments: initial, focused, time-lapsed and emergency.
What is history taking of a patient?
The method by which doctors gather information about a patient’s past and present medical condition in order to make informed clinical decisions is called the history and physical (a.k.a. the H&P).
How do you take clinical history of a patient?
- Introduce yourself, identify your patient and gain consent to speak with them. …
- Step 02 – Presenting Complaint (PC) …
- Step 03 – History of Presenting Complaint (HPC) …
- Step 04 – Past Medical History (PMH) …
- Step 05 – Drug History (DH) …
- Step 06 – Family History (FH) …
- Step 07 – Social History (SH)
How do I do a health history assessment?
- Biographical data. Source of history. …
- Reason for seeking care and history of present health concern. Chief complaint. …
- Past health history. Allergies (reaction) …
- Family history. …
- Functional assessment (including activities of daily living) …
- Developmental tasks. …
- Cultural assessment.
What is a health history questionnaire?
A health history questionnaire consists of a set of survey questions that help either medical researcher, doctors or medical professional, hospitals or small clinics to understand the population they provide medical services to. … To treat a patient optimally a doctor must know the details of his/her medical history.
Why is health history important in nursing?
Taking a comprehensive health history is a core competency of the advanced nursing role. The purpose of the health history is to source important and intimate knowledge about the patient and allow the nurse and patient to establish a therapeutic relationship.
What are health history questions?
- What countries did our relatives come from?
- Did our late relatives have health problems? What were the issues and when were they diagnosed?
- How old were they when they died?
- What were the reasons for their deaths?
Why is it important to obtain a complete description of the patient's past medical history?
This information gives your doctor all kinds of important clues about what’s going on with your health, because many diseases run in families. The history also tells your doctor what health issues you may be at risk for in the future.
What are the 5 nursing process?
The nursing process functions as a systematic guide to client-centered care with 5 sequential steps. These are assessment, diagnosis, planning, implementation, and evaluation.
What is an example of a nursing diagnosis?
An example of an actual nursing diagnosis is: Sleep deprivation. Describes human responses to health conditions/life processes that may develop in a vulnerable individual/family/community. It is supported by risk factors that contribute to increased vulnerability. An example of a risk diagnosis is: Risk for shock.
How do you ask a patient about social history?
- What other health care professionals are currently helping care for you?
- What are your average daily activities?
- Any children? …
- Ethnic background?
- Finances; home situation (location, suitability, help available, transportation)
- What do you do for a living?
- Any inherited diseases?
How do you summarize a patient's history?
Summarising. After taking the history, it’s useful to give the patient a run-down of what they’ve told you as you understand it. For example: ‘So, Michael, from what I understand you’ve been losing weight, feeling sick, had trouble swallowing – particularly meat – and the whole thing’s been getting you down.
What should be included in history of present illness?
- Location: What is the location of the pain?
- Quality: Include a description of the quality of the symptom (i.e. sharp pain)
- Severity: Degree of pain for example can be described on a scale of 1 – 10.
- Duration: How long have you had the pain.
What are the four elements of history?
The four recognized levels of history are problem-focused, expanded problem-focused, detailed, and comprehensive. The number of elements documented in the progress note determines level selection.