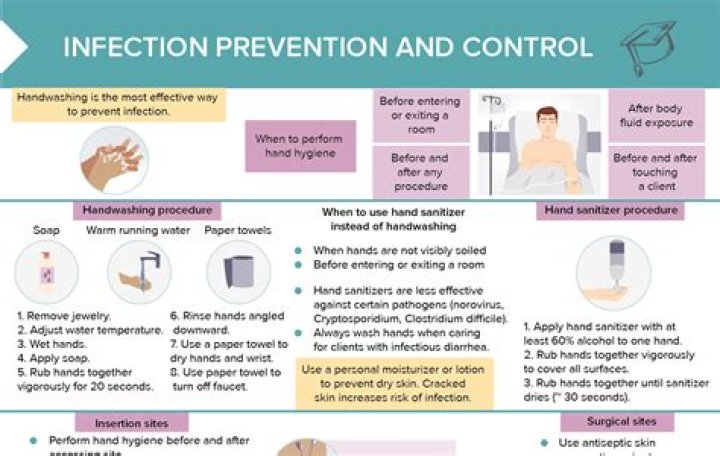
What are the core activities of an infection prevention and control program
 Christopher Lucas
Christopher Lucas An IPC program should be implemented multimodally, i.e. using an integrated approach with several components. Common components are system change, education and training, monitoring and feedback, reminders, and culture change.
What are the basic principles of infection prevention and control?
- Introduction. …
- The general principles of infection prevention and control. Hand hygiene.
- Using personal protective equipment. …
- Safe handling and disposal of sharps. Safe handling and disposal of chemical waste.
- Managing blood and bodily fluids.
What are IPC Programmes?
What is Integrated Personal Commissioning (IPC)? Integrated Personal Commissioning (IPC) is a nationally led, locally delivered programme that is supporting healthcare empowerment and the better integration of services across health, social care and the voluntary and community sector.
What are the 5 standard precautions for infection control?
- Hand hygiene.
- Use of personal protective equipment (e.g., gloves, masks, eyewear).
- Respiratory hygiene / cough etiquette.
- Sharps safety (engineering and work practice controls).
- Safe injection practices (i.e., aseptic technique for parenteral medications).
- Sterile instruments and devices.
What is an infection control program?
Infection control refers to the policy and procedures implemented to control and minimize the dissemination of infections in hospitals and other healthcare settings with the main purpose of reducing infection rates.
What is the role of the infection prevention and control team?
The role of the Infection Prevention & Control Team (IP&CT) is to promote best infection control practice in order to ensure the delivery of a quality service for patients, visitors and staff. The IP&CT do this by: • Providing advice on management of patients with infections.
What are the 10 standard infection control precautions?
- 1.1 Patient Placement/Assessment for infection risk.
- 1.2 Hand Hygiene.
- 1.3 Respiratory and Cough Hygiene.
- 1.4 Personal Protective Equipment.
- 1.5 Safe Management of Care Equipment.
- 1.6 Safe Management of Care Environment.
- 1.7 Safe Management of Linen.
- 1.8 Safe Management of Blood and Body Fluid Spillages.
How do you ensure infection control?
- Continually educate staff. …
- Set clear processes and policies. …
- Create a cleanliness culture. …
- Hold regular audits.
What are the four major methods of infection control?
- hand hygiene and cough etiquette.
- the use of personal protective equipment (PPE)
- the safe use and disposal of sharps.
- routine environmental cleaning.
- incorporation of safe practices for handling blood, body fluids and secretions as well as excretions [91].
- Wash your hands well. …
- Cover a cough. …
- Wash and bandage all cuts. …
- Do not pick at healing wounds or blemishes, or squeeze pimples.
- Don’t share dishes, glasses, or eating utensils.
- Avoid direct contact with napkins, tissues, handkerchiefs, or similar items used by others.
What is core infection?
Co-infection is the simultaneous infection of a host by multiple pathogen species, for instance multi-parasite infections. Co-infection also occurs as simultaneous infection of a single cell by two or more virus particles, which can arise incrementally by initial infection followed by superinfection.
What is the most essential component of an effective infection prevention surveillance program is?
key elements (e.g., governance, policy/pro- cedure, education/training, surveillance, and monitoring of hospital hygiene) have been identified as essential components of an IPC program and should be addressed by all services (Figure 1).
What are the 5 moments of hand hygiene?
- The 5 Moments.
- Moment 1 – before touching a patient.
- Moment 2 – before a procedure.
- Moment 3 – after a procedure or body fluid exposure risk.
- Moment 4 – after touching a patient.
- Moment 5 – after touching a patient’s surroundings.
What are 3 ways to reduce possible spread of infection?
- Immunise against infectious diseases.
- Wash and dry your hands regularly and well.
- Stay at home if you are sick.
- Cover coughs and sneezes.
- Clean surfaces regularly.
- Ventilate your home.
- Prepare food safely.
- Practise safe sex.
What are the standard precautions for infection prevention and control which affect your own practice in preparing and dressing for work?
Standard precautions consist of eight key elements. These include correct hand hygiene, safe cleaning and decontamination, safe handling and disposal of waste and linen, sharps safety, correct use of personal protective clothing, safe handling of blood and body fluids and respiratory hygiene.
What are the two basic goals of infection control?
The two basic goals of infection control are to protect the patient and health care personnel from infection. Infection control starts with standard precautions. Standard precautions are the methods recommended by the Centers for Disease Control and Prevention (CDC) for preventing the transmission of infections.
What does an infection prevention and control nurse do?
The basic role of the IPC Nurse is to ensure that Healthcare Acquired Infections (HCAIs) are prevented and where unable to prevent infections, control measures are put in place to stop or minimise the spread of infections.
What is the first step in the infection prevention and control process?
The first step in infection control is hand hygiene.
What are the stages of infection control?
The six links include: the infectious agent, reservoir, portal of exit, mode of transmission, portal of entry, and susceptible host. The way to stop germs from spreading is by interrupting this chain at any link.
Why is infection prevention and control important in the practice of Venepuncture?
Venepuncture is the procedure of entering a vein with a needle in order to obtain a sample of blood for diagnostic purposes. Venepuncture breaches the circulatory system, therefore, to minimise the risk of injury and/or infection to both staff and patients, standard precautions should be adhered to.
What is the meaning of super infection?
Medical Definition of superinfection : a second infection superimposed on an earlier one especially by a different microbial agent of exogenous or endogenous origin that is resistant to the treatment used against the first infection.
What are secondary infections?
A secondary infection is an infection that occurs during or after treatment for another infection. It may be caused by the first treatment or by changes in the immune system. Two examples of a secondary infection are: A vaginal yeast infection after taking antibiotics to treat an infection caused by bacteria.
What is aseptic technique CDC?
Aseptic technique means using practices and procedures to prevent contamination from pathogens. It involves applying the strictest rules to minimize the risk of infection. Healthcare workers use aseptic technique in surgery rooms, clinics, outpatient care centers, and other health care settings.
What must be the composition of an effective hospital infection control team?
The basic components for successful hospital infection control include: (1) personnel and supporting resources proportional to size, complexity and estimated risk of the population served; (2) trained hospital infection control practitioners; and (3) the necessary structure to implement changes in medical, nursing and …
Why is hand washing important in infection control?
Germs from unwashed hands can be transferred to other objects, like handrails, table tops, or toys, and then transferred to another person’s hands. Removing germs through handwashing therefore helps prevent diarrhea and respiratory infections and may even help prevent skin and eye infections.
What are the six steps of hand washing?
- Wash palms of hands.
- Wash between fingers at back of hands.
- Wash between fingers palm to palm.
- Wash palm area.
- Pay particular attention to thumb area and thumb joint.
- Wash finger tips paying particular attention to nails and dry hands well with clean disposable towel discarding correctly.
How do risk assessments help prevent the spread of infections?
Risk assessments help organisations to identify potential hazards and react to them before they cause an outbreak of infection or disease. This protects the health and safety of the organisation’s employees and the people that they then encounter.
What are the three elements required to spread an infection?
Transmission of infectious agents within a healthcare setting requires three elements: a source (or reservoir) of infectious agents, a susceptible host with a portal of entry receptive to the agent, and a mode of transmission for the agent.
What is the most effective way of preventing cross infection?
Hand hygiene is one of the most simple but effective means of preventing the spread of infections. You should always wash your hands when entering and before leaving a ward, when you have used the toilet, bedpan or commode and before eating or drinking.
What is the most effective method of preventing communicable disease?
Keeping personal hygiene, like taking a daily bath and washing your hands frequently. Hand washing with soap and water is the simplest and one of the most effective ways to prevent transmission of many communicable diseases (Figure 2.5).