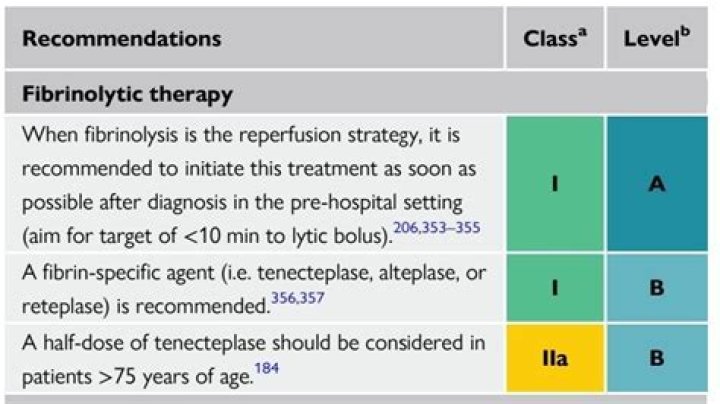
Which finding would exclude your patient from receiving Fibrinolytics?
 Emily Sparks
Emily Sparks .
Regarding this, what are contraindications to fibrinolytic therapy?
Relative contraindications (not absolute) to fibrinolytic therapy include: Intracranial abnormality not listed as absolute contraindication (i.e. benign intracranial tumor) Ischemic stroke more than 3 months prior. Bleeding within 2 to 4 weeks (excluding menses)
One may also ask, what is fibrinolytic checklist? Fibrinolytic therapy is the treatment of choice for STEMI patients who meet specific criteria: Patient has been symptomatic (Chest pain) for longer than 15 minutes but less than 12 hours. ECG is diagnostic for ST elevation indicating an MI or a new Left Bundle Branch Block.
Subsequently, question is, what are the guidelines for antiplatelet and fibrinolytic therapy?
Do not give anticoagulants or antiplatelet treatment for 24 hours after tPA until a follow-up CT scan at 24 hrs does not show intracranial hemorrhage. If the patient is NOT a candidate for fibrinolytic therapy, give the patient aspirin.
Who Cannot receive tPA?
If the patient has an elevated blood pressure (SBP >185 or DBP >110) as their only contraindication to receiving tPA, consider using parenteral medication to lower their blood pressure to an acceptable level.
Related Question AnswersWhen should you not use tPA?
Contraindications for IV tPA:- ? Symptom onset is unknown, > 4.5 hours, or if patient awoke with stroke.
- ? Acute or previous intracranial hemorrhage.
- ? Imaging showing extensive regions of irreversible injury (hypoattenuation)
- ? Prior ischemic stroke, severe head trauma, or intracranial/intraspinal surgery within 3 months.
What is the most common complication following an AMI?
Complications of AMI include: Ischaemic (including failure of reperfusion): angina, re-infarction, infarct extension. Mechanical: heart failure, cardiogenic shock, mitral valve dysfunction, aneurysms, cardiac rupture. Arrhythmic: atrial or ventricular arrhythmias, sinus or atrioventricular (AV) node dysfunction.What are examples of Fibrinolytics?
The most commonly used clot-busting drugs -- also known as thrombolytic agents -- include:- Eminase (anistreplase)
- Retavase (reteplase)
- Streptase (streptokinase, kabikinase)
- t-PA (class of drugs that includes Activase)
- TNKase (tenecteplase)
- Abbokinase, Kinlytic (rokinase)
Can nurses give tPA?
To be eligible for tPA, the patient must reach a certified stroke center as soon as possible after symptom onset. As a nurse, your assessment of the patient's signs and symptoms and your knowledge of stroke treatment are vital.What is the process of fibrinolysis?
Fibrinolysis. In fibrinolysis, a fibrin clot, the product of coagulation, is broken down. Its main enzyme plasmin cuts the fibrin mesh at various places, leading to the production of circulating fragments that are cleared by other proteases or by the kidney and liver.Is aspirin a fibrinolytic?
Aspirin and fibrinolysis Although it is well known that aspirin (ASA) decreases platelets activity and possesses antithrombotic action, its effect on fibrinolysis has not been yet entirely established.How long does it take for tPA to work?
Administration of tPA Treatment with tissue plasminogen activator (tPA) has been effective for people with an ischemic stroke as long as it is received intravenously within three hours of the onset of symptoms.Is Heparin a fibrinolytic?
Fibrinolytic drugs work by activating the so-called fibrinolytic pathway. This distinguishes them from the anticoagulant drugs (coumarin derivatives and heparin), which prevent the formation of blood clots by suppressing the synthesis or function of various clotting factors that are normally present in the blood.What is the stroke protocol?
Assoc Prof Frank Gaillard ? ? and Dr Bruno Di Muzio ? et al. MRI protocol for stroke assessment is a group of MRI sequences put together to best approach brain ischemia. Some institutions also apply a quick MRI stroke protocol for code stroke patients assessment within the narrow time window for thrombolytic therapy.What drugs are used in ACLS?
ACLS, PALS, and BLS Drug Guide- Adenosine. Amiodarone. Atropine. Diltiazem.
- Dopamine. Epinephrine. Lidocaine. Magnesium.
- Naloxone. Procainamide. Sotalol. Adjunct Medications. Isoproterenol.
Which patient is a candidate for fibrinolytic therapy?
Fibrinolytic therapy works by dissolving clots which are obstructing blood flow to the brain. In order to be considered a suitable candidate for the therapy, patients must be over the age of 18 and have a firm diagnosis of ischemic stroke with deficits.Which intervention is most appropriate for the treatment of a patient in asystole?
The only 2 drugs recommended or acceptable by the American Heart Association (AHA) for adults in asystole are epinephrine and vasopressin. Atropine is no longer recommended for young children and infants since 2005, and for adults since 2010 for pulseless electrical activity (PEA) and asystole.What test should be performed before administering tPA?
Ischemic Stroke: The only blood test that should be done before tPA usage is the blood glucose level. If the patient is on anticoagulation like coumadin then only we should do PT, PTT, and INR etc. The benefit of tPA depends a lot on time.What is fibrinolytic therapy drugs?
There are three major classes of fibrinolytic drugs: tissue plasminogen activator (tPA), streptokinase (SK), and urokinase (UK). While drugs in these three classes all have the ability to effectively dissolve blood clots, they differ in their detailed mechanisms in ways that alter their selectivity for fibrin clots.Is aspirin contraindicated with tPA?
However, it should be noted that pre-TPA aspirin use was not associated with an increased ICH risk in patients given the drug (16) and therefore pre-morbid aspirin use is not considered a contraindication for TPA administration in acute stroke.Can you give tPA after aspirin?
As with IV tPA, treatment with mechanical thrombectomy should be initiated as quickly as possible. Administration of aspirin is recommended in acute stroke patients within 24-48 hours after stroke onset. For patients treated with IV tPA, aspirin administration is generally delayed for 24 hours.How effective is Thrombolysis in Stroke?
Setting up a thrombolysis service There is evidence of benefit for thrombolysis up to 4.5 h after the onset of stroke symptoms, but patients who receive thrombolysis within 90 min receive twice as much benefit as patients who receive thrombolysis between 3 and 4.5 h [Hacke et al.Why is a fibrinolytic checklist for stemi done?
Fibrinolytic checklist. Fibrinolysis can be effective for the treatment of ST-segment elevation myocardial infarction. The medication can dissolve the thrombus/embolus that is lodged in a coronary artery, thus restoring blood flow to the heart.How do you administer thrombolytics?
SYSTEMIC THROMBOLYSIS is used for heart attack, stroke and pulmonary embolism.- The “clot-busting” drug will be delivered through a peripheral intravenous (IV) line, usually through a visible vein in your arm.
- Performed at your bedside in an intensive care unit while your heart and lung functions are monitored.





