Which artificial airway is used for long term airway
 Emily Sparks
Emily Sparks Which artificial airway is used for long-term airway management?a.Tracheostomy tubeb.Nasopharyngeal airwayc.Endotracheal tubed.Laryngeal mask airway (LMA)
Which is the most suitable method for long term management of airway?
The most widely used route is orotracheal, in which an endotracheal tube is passed through the mouth and vocal apparatus into the trachea.
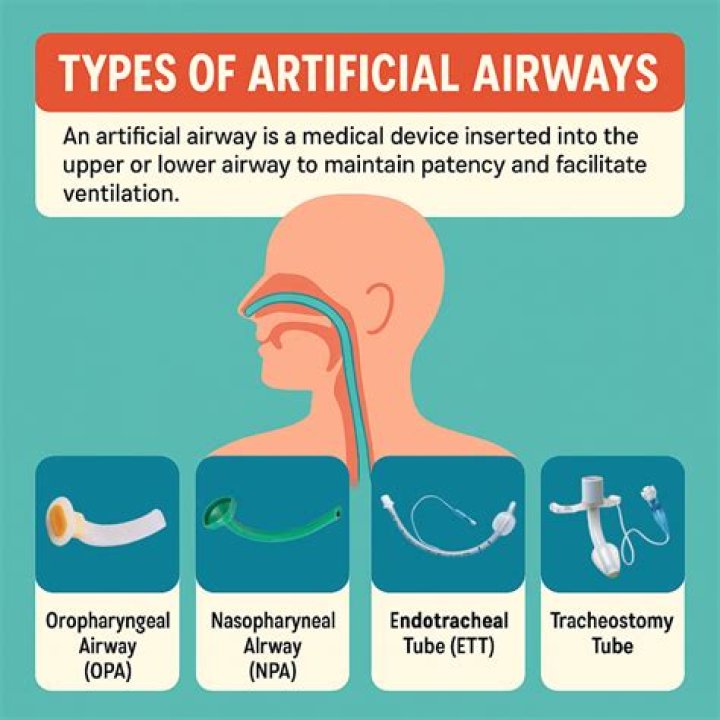
What are the types of artificial airway?
- oropharyngeal.
- nasopharyngeal.
- endotracheal.
- laryngeal mask airway.
- cricothyroidotomy.
- tracheostomy.
What are the 3 types of artificial airways?
Artificial airways include endotracheal, tracheotomy, and laryngectomy tubes [1]. Mechanical ventilation may be necessary for any patients for whom the process of ventilation has been significantly altered.What is considered long term intubation?
Prolonged intubation is defined as intubation exceeding 7 days [25]. Clinical studies have shown that prolonged intubation is a risk factor for many complications.
Who needs to intubate?
Indications for intubation to secure the airway include respiratory failure (hypoxic or hypercapnic), apnea, a reduced level of consciousness (sometimes stated as GCS less than or equal to 8), rapid change of mental status, airway injury or impending airway compromise, high risk for aspiration, or ‘trauma to the box ( …
What is RSI EMS?
OVERVIEW. Rapid sequence intubation (RSI) is an airway management technique that produces inducing immediate unresponsiveness (induction agent) and muscular relaxation (neuromuscular blocking agent) and is the fastest and most effective means of controlling the emergency airway.
What are types of airway management?
The five types include facemask ventilation devices, which may use additional attachments; supraglottic airway devices; tracheal intubation; suction machines for airway clearance; and transtracheal access.When do you use advanced airway?
- Traumatic airway injury.
- Apnea.
- Hypoxia.
- Change of mental status or reduced consciousness.
- High aspiration risk.
- Penetrating abdominal or chest injuries.
The laryngeal tube (also known as the King LT) is an airway management device designed as an alternative to other airway management techniques such as mask ventilation, laryngeal mask airway, and tracheal intubation.
Article first time published onWhat is I gel airway?
The i-gel, invented by Muhammed Aslam Nasir, is a new supraglottic airway, consisting of a mask and a tube. One notable feature of the i-gel is that the rim of the mask is designed to conform to the anatomical shape of the larynx. This enables the device to provide an airtight seal without the cuff mechanism.
What is the medical term for airway?
Medical Definition of airway : a passageway for air into or out of the lungs specifically : a device passed into the trachea by way of the mouth or nose or through an incision to maintain a clear respiratory passageway (as during anesthesia, convulsions, or in obstructive laryngitis) — see upper airway.
What is the difference between tracheostomy and intubation?
An endotracheal tube is an example of an artificial airway. A tracheostomy is another type of artificial airway. The word intubation means to “insert a tube”. Usually, the word intubation is used in reference to the insertion of an endotracheal tube (Image 1).
What's the difference between intubation and ventilation?
Intubation is placing a tube in your throat to help move air in and out of your lungs. Mechanical ventilation is the use of a machine to move air in and out of your lungs.
Why is a trach better than a ventilator?
Tracheostomy is thought to provide several advantages over translaryngeal intubation in patients undergoing PMV, such as the promotion of oral hygiene and pulmonary toilet, improved patient comfort, decreased airway resistance, accelerated weaning from mechanical ventilation (MV) [4], the ability to transfer ventilator …
Is etomidate a paralytic?
Etomidate, when used in paralytic RSI, is pushed as rapidly as possible and is immediately followed by the neuromuscular blocking agent. This medication sequence renders the patient almost instantly unconscious and paralyzed.
Why is succinylcholine used in RSI?
RSI is an anesthesia induction technique designed to facilitate rapid tracheal intubation in patients at high risk for pulmonary aspiration. Succinylcholine has been a mainstay of RSI for more than 50 years, primarily because of the drug’s rapid onset time.
How fast do you push succinylcholine?
The dose of succinylcholine administered by infusion depends upon the duration of the surgical procedure and the need for muscle relaxation. The average rate for an adult ranges between 2.5 and 4.3 mg per minute.
What is the difference between a ventilator and a respirator?
Your doctor might call it a “mechanical ventilator.” People also often refer to it as a “breathing machine” or “respirator.” Technically, a respirator is a mask that medical workers wear when they care for someone with a contagious illness. A ventilator is a bedside machine with tubes that connect to your airways.
Is intubation permanent?
Intubation is a standard procedure that involves passing a tube into a person’s airway. Doctors often perform it before surgery or in emergencies to give medicine or help a person breathe. Most people recover from intubation with no long-term effects.
Is it painful to be intubated?
Intubation is an invasive procedure and can cause considerable discomfort. However, you’ll typically be given general anesthesia and a muscle relaxing medication so that you don’t feel any pain. With certain medical conditions, the procedure may need to be performed while a person is still awake.
Can a nurse place an LMA?
The LMA has been successfully used by nurses during cardiopulmonary resuscitation (Baskett, 1994). Ventilation using a bag/valve/LMA device is more efficient, and certainly easier, than the conventional bag/valve/mask device, and the incidence of regurgitation is lower (Resuscitation Council (UK), 2000).
What is the difference between LMA and ETT?
Conclusion: The LMA does not provide safe patent airway to facilitate bedside PDT in critically sick population on controlled ventilation. The ETT is safer for controlled ventilation and should be continued to secure the airway for this purpose until a better alternative is available.
How long can LMA stay in?
The laryngeal mask airway (LMA) has been used successfully in numerous cases since its introduction more than 30 years ago. While some contraindications to LMA use are absolute others are less well defined. An upper time limit of three hours has been recommended for patients whose airway is managed with an LMA.
Is an LMA an advanced airway?
The laryngeal mask airway (LMA) is an advanced airway alternative to ET intubation and provides comparable ventilation. It is acceptable to use the LMA as an alternative to an esophageal-tracheal tube for airway management in cardiac arrest.
What are supraglottic airway devices?
Supraglottic airways (SGAs) are a group of airway devices that can be inserted into the pharynx to allow ventilation, oxygenation, and administration of anesthetic gases, without the need for endotracheal intubation.
Is a King airway considered an advanced airway?
Other advanced airways include supraglottic airways like the Combitube, King Airway, LMA, and the new iGel. These devices may be just as detrimental to the patient if improperly placed. However, they may provide equal airway management in certain patients and allow chest compressions to continue without interruption.
What is advanced airway in CPR?
When an advanced airway (ie, endotracheal tube, Combitube, or LMA) is in place during 2-person CPR, ventilate at a rate of 8 to 10 breaths per minute without attempting to synchronize breaths between compressions. There should be no pause in chest compressions for delivery of ventilations (Class IIa).
How do you maintain an airway?
Techniques to open and clear the airway Head tilt, chin lift and jaw thrust are three manoeuvres that can improve patency of the airway, which may have been obstructed by the tongue or other upper airway structures such as the soft palate and epiglottis (Nolan et al 2005).
When is a King LT used?
1 Goal/Purpose/Description 1.1 The King Airway (LT-D) is to be used as an alternative to endotracheal intubation for advanced airway management 1.2 It is placed in the esophagus and serves as a mechanical airway when ventilation is needed for patients who are over 4 feet tall and apneic or unconscious with ineffective …
Is Combitube a supraglottic airway?
The esophageal tracheal combitube (ETC) is a supraglottic airway device that functions as an effective alternative to ventilation via mask and tracheal intubation and is therefore a valuable tool in difficult and emergency airway management.