What is the purpose of the inner cannula on a tracheostomy
 Christopher Lucas
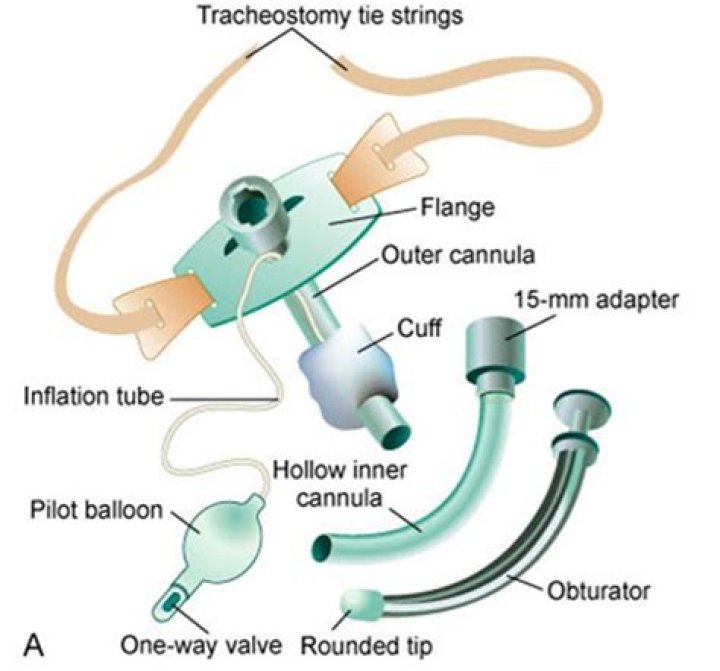
Christopher Lucas Tracheostomy tubes often have an ‘inner cannula’ or ‘inner tube’. This is a tube within the outer tube which can be removed and cleaned easily, without having to change the whole (outer) tracheostomy tube. Inner cannulae do narrow the tracheotomy tube which can make it harder to breathe through.
Why is there an inner cannula for tracheostomy?
Inner Cannula: The inner cannula fits inside the trach tube and acts as a liner. This liner can be removed and cleaned to help prevent the build-up of mucus inside the trach tube. The inner cannula locks into place to prevent accidental removal.
How often do you change a trach inner cannula?
The tracheostomy inner cannula tube should be cleaned two to three times per day or more as needed. Please note that this only applies to reusable inner cannulas.
What is the difference between the inner and outer cannula for a tracheostomy?
The outer cannula is the outer tube that holds the tracheostomy open. … The inner cannula fits inside the outer cannula. It has a lock to keep it from being coughed out, and it is removed for cleaning. The obturator is used to insert a tracheostomy tube.Can you suction without an inner cannula?
If the patient has a fenestrated tracheostomy tube, the unfenestrated inner cannula must be in place before suctioning.
What is the difference between a cuffed and uncuffed Trach?
Tracheostomy tubes can be cuffed or uncuffed. Uncuffed tubes allow airway clearance but provide no protection from aspiration. Cuffed tracheostomy tubes allow secretion clearance and offer some protection from aspiration, and positive-pressure ventilation can be more effectively applied when the cuff is inflated.
What is the difference between an endotracheal tube and a tracheostomy?
An endotracheal tube is an example of an artificial airway. A tracheostomy is another type of artificial airway. The word intubation means to “insert a tube”.
Does a cuffed trach prevent aspiration?
The definition of aspiration is when any food, liquid, or other matter passes below the vocal folds. Therefore, the cuff cannot prevent aspiration as it is located below the vocal folds.Does cuffed trach have inner cannula?
3.9): These plastic tubes (uncuffed and cuffed) do not have inner cannulae. The outer cannula has a 15 mm adaptor. Available in multiple sizes.
How do you tell if a trach is cuffed?If the tracheostomy tube has a pilot line and pilot balloon, this is an indicator that the patient has a cuffed tracheostomy tube. The flange of the tracheostomy tube also indicates if the tracheostomy tube has a cuff in place. When the pilot balloon is inflated, this indicates that the cuff is inflated.
Article first time published onHow many times can you reuse an inner cannula?
– 2 clean or sterile bowls- Hydrogen peroxide- Tongs or tweezers- Gloves- Several sterile gauze packets – one to store cleaned inner cannula
How do you dry an inner cannula on a tracheostomy tube?
Place the soiled inner cannula in a small clean bowl containing sterile water. Allow to soak and then use a small, non- abrasive brush to gently remove the mucus. Air dry the inner cannula by gently shaking it. After cleaning, rinse the inner cannula thoroughly with sterile water.
Does Trach suctioning need to be sterile?
Aseptic or clean techniques may be used for auctioning. An aseptic technique requires the use of sterile gloves and a sterile catheter. The clean technique does not require a sterile glove, and the pupil’s same catheter may be used throughout the school day.
How far down do you suction a tracheostomy?
s tracheostomy tube is 4 cm long, place the catheter 4 cm into the tracheostomy tube. Often, there will be instances when this technique of suctioning (called tip suctioning) will not clear the patient? s secretions.
How often should a patient with a tracheostomy tube be suctioned?
Suction the trach 3 to 4 times a day, or more if needed. For example, two of the times could be before you go to bed and when you wake up in the morning. You will need suction catheters, a suction machine, saline fluid, a small cup, and a mirror.
What is the normal tracheostomy cuff pressure?
The pressure within the cuff should be checked regularly with a handheld pressure manometer and maintained ideally between 20 and 25 cm water. It should never exceed 25 cm water. If an air leak occurs with the cuff pressure at the maximum recommended, the tracheostomy may have become displaced and may require changing.
Why use an LMA over an ETT?
The LMA has many advantages over an ET tube in that LMAs are less invasive, decrease airway trauma, decrease neck mobility requirements, and have a reduced risk of laryngospasm and bronchospasm.
Can you intubate a patient with a tracheostomy?
If the trach is less than 7 days old, prepare for oral intubation and contact ENT. Oral intubation can be done if the upper airway is patent. Cover the stoma site after intubation. If the upper airway is obstructed or anatomy abnormal, prepare for difficult airway (Cric set, fiberoptic), and call ENT.
What is one advantage of a tracheostomy tube over an endotracheal tube?
The benefits of tracheostomy over translaryngeal intubation includes improved patient comfort, better oral hygiene, less dental damage and tracheal injury, easier and safer nursing care, and lower airway resistance, which may facilitate the weaning process and avoid ventilator-associated pneumonia8.
When would you use an uncuffed tracheostomy?
An uncuffed tube is suitable for a patient in the recovery phase of critical illness who has returned from intensive care and may still require chest physiotherapy, suction via the trachea and airway support.
What is capping a tracheostomy?
A commonly used test to determine whether a critically ill patient with a tracheostomy tube is ready for decannulation is a capping trial, in which a cap is placed over the tracheostomy tube for a period of time to see whether the patient is able to breathe around the tracheostomy tube (or through a fenestration in the …
Can you talk with an uncuffed Trach?
Because air no longer passes over the vocal cords, speech isn’t possible. An uncuffed tube may permit limited speech, if enough air circulates around the tube to permit the patient to say a word or two. However, speaking with an uncuffed tube increases the patient’s work of breathing.
What is the pilot balloon on a tracheostomy?
The pilot balloon port is attached to tubing that inflates the cuff at the base of the tracheostomy tube to hold it in place within the trachea. The balloon inflates along with the cuff and serves as an indication of how much air pressure is in the cuff.
When will the cuff be inflated on a tracheostomy tube?
Inflate cuff 24 hours following initial tracheostomy tube placement (prevents accumulation of subcutaneous air and aspiration of secretions) Manual assisted ventilation/mechanical ventilation. Meals or nasogastric tube feedings for 30 minutes after if problems with aspiration are anticipated.
Can you aspirate if you are intubated?
BACKGROUND: Pulmonary aspiration of gastric contents during tracheal intubation is a life-threatening complication in emergency patients. Rapid sequence intubation is commonly performed to prevent aspiration but is not associated with low risk of intubation related complications.
What is the most serious complication of a tracheostomy?
Bleeding. Air trapped around the lungs (pneumothorax) Air trapped in the deeper layers of the chest(pneumomediastinum) Air trapped underneath the skin around the tracheostomy (subcutaneous emphysema) Damage to the swallowing tube (esophagus)
When do you use Passy Muir valve?
The Passy-Muir speaking valve is commonly used to help patients speak more normally. This one-way valve attaches to the outside opening of the tracheostomy tube and allows air to pass into the tracheostomy, but not out through it. The valve opens when the patient breathes in.
How often should inner cannula be changed at home?
Secretions can adhere to the inner cannula which can reduce the inner diameter resulting in increased work of breathing and potentially block the patient’s airway. The inner cannula should be removed and inspected once per 8 hour shift or if the patient shows any signs of respiratory distress.
Can you vomit with a tracheostomy?
If you vomit, cover the tracheostomy tube with an artificial nose or towel to keep vomit out of your airway. If you think vomit may have entered the tracheostomy tube, suction immediately. Be sure to drink plenty of fluids, particularly if you have fever, vomiting, or diarrhea. Watch for signs of infection.
What is the quality of life after a tracheostomy?
The median survival after tracheostomy was 21 months (range, 0-155 months). The survival rate was 65% by 1 year and 45% by 2 years after tracheostomy. Survival was significantly shorter in patients older than 60 years at tracheostomy, with a hazard ratio of dying of 2.1 (95% confidence interval, 1.1-3.9).
What size inner cannula do you obtain for trach Care?
15mm connector – part of the tracheostomy tube or inner cannula that sticks out at the neck. Ventilator tubing, a manual resuscitation bag, or a speaking valve may be connected to the 15mm connector.