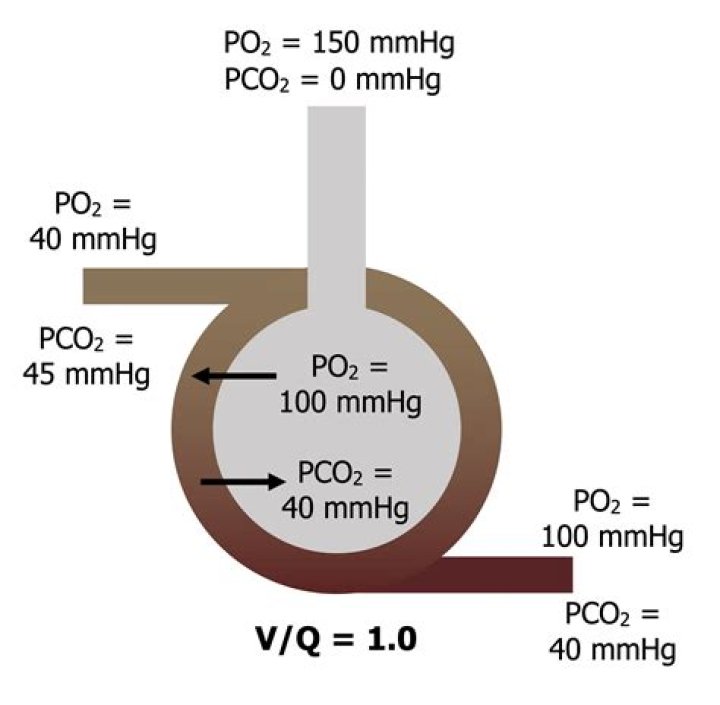
What is po2 and pCO2 in the alveolar cavity
 Isabella Bartlett
Isabella Bartlett 1) PO2 in alveoli is 104 mmHg vs. 40 mmHg for the deoxygenated blood of the pulmonary arteries. … 2) PCO2 in alveoli is at 40 mmHg vs. 45 mmHg in blood returning from tissues.
What is the PO2 of alveolar gas?
For example, at sea level with no additional supplemental oxygen and a normal physiological state, the PO2 inside the alveoli calculates at approximately 100 mm Hg. But, if a patient is given 100% oxygen in the same situation the PO2 can be as high as 663 mm Hg.
What is the PO2 in the lungs?
PO2 (partial pressure of oxygen) reflects the amount of oxygen gas dissolved in the blood. It primarily measures the effectiveness of the lungs in pulling oxygen into the blood stream from the atmosphere. Elevated pO2 levels are associated with: Increased oxygen levels in the inhaled air.
What will be the PO2 and PCO2 in the alveolar air compared to those in the dead space air?
In atmospheric air, pO2 is about 159 mm Hg. In alveolar air, it is about 104 mm Hg. The partial pressure of carbon dioxide in atmospheric air is lesser than that of carbon dioxide in alveolar air. In atmospheric air, pCO2 is about 0.3 mmHg.How is PO2 calculated in alveoli?
The alveolar gas equation is of great help in calculating and closely estimating the partial pressure of oxygen inside the alveoli. The alveolar gas equation is used to calculate alveolar oxygen partial pressure: PAO2 = (Patm – PH2O) FiO2 – PACO2 / RQ.
What will be the PO2 and PCO2 in the atmospheric air?
In atmospheric air, pO2 is about 159 mm Hg. In alveolar air, it is about 104 mm Hg. The partial pressure of carbon dioxide in atmospheric air is lesser than that of carbon dioxide in alveolar air. In atmospheric air, pCO2 is about 0.3 mmHg.
Is PO2 and PaO2 the same?
PO2 is just partial pressure of oxgen in a given environment, such as room air. … PAO2 is partial pressure of oxygen in alveoli. PaO2 is partial pressure of oxygen dissolved in (arterial) blood. Partial pressure of a gas dissolved in a liquid depends on the qualities of the liquid and the concentration of the gas.
What is PO2 and PCO2 in systemic arteries?
The amount of oxygen that can bind with haemoglobin is determined by oxygen tension. This is expressed as partial pressure of oxygen pO2, similarly partial pressure of carbon dioxide is pCO2. The pCO2 and pO2 in oxygenated blood i.e., arterial blood is 40 mm Hg and 95 mm Hg respectively.Why is the PO2 of alveolar air significantly lower than the PO2 of atmospheric air?
Partial pressures The alveolar oxygen partial pressure is lower than the atmospheric O2 partial pressure for two reasons. … The rest of the difference is due to the continual uptake of oxygen by the pulmonary capillaries, and the continual diffusion of CO2 out of the capillaries into the alveoli.
What is the PO2 of alveolar air quizlet?no alveolar ventilation = air in alveolus comes to equilibrium with blood O2 and CO2, so alveoli without ventilation will have PO2 = 40 and PCO2 = 45 mmHg.
Article first time published onWhat does a low PCO2 mean?
The pCO2 gives an indication of the respiratory component of the blood gas results. A high and low value indicates hypercapnea (hypoventilation) and hypocapnea (hyperventilation), respectively. A high pCO2 is compatible with a respiratory acidosis and a low pCO2 with a respiratory alkalosis.
What increases alveolar PO2?
Which of the following will increase alveolar PO2 ? -An increase in alveolar P O2 results from an increase in alveolar ventilation (supply of oxygen) relative to metabolic rate (consumption of oxygen). systemic arterial oxygen saturation in the blood? curve—a P O2 of between 40 and 60 mmHg.
How do you find PO2?
P divided by F = P/F ratio. Example: PaO2 = 90 on 40% oxygen (FIO2 = 0.40): 90 / 0.40 = P/F ratio = 225. A P/F ratio of 225 is equivalent to a pO2 of 45 mmHg, which is significantly < 60 mmHg on room air.
How do you calculate alveolar PCO2?
- PACO2 = V’CO2/V’A
- PACO2 = Alveolar Partial Pressure of CO2
- V’CO2 = Metabolic Rate of CO2 production.
- V’A = Alveolar Ventilation (ml/min)
Is PaCO2 and PCO2 the same?
Probably the most common usage of PCO2 is the measuring of PaCO2 from arterial blood or PvCO2 from venous blood. … It is the change in local PaCO2 as well as the change in pH that causes a change in minute ventilation.
What is SaO2 vs SpO2?
Pulse oximeters measure blood oxygen saturation noninvasively and continu- ously. What is SpO2? A blood-oxygen saturation reading indicates the percentage of hemoglobin molecules in the arterial blood which are saturated with oxygen. The reading may be referred to as SaO2.
What is PaO2 SaO2 and SpO2?
SpO2 = oxygen saturation as measured by pulse oximeter. SaO2 = oxygen saturation as measured by blood analysis (e.g. a blood gas) PaO2 = partial pressure of oxygen in the blood, as measured by blood analysis. .dyspnea.
What happens when PO2 is low?
If a PaO2 level is lower than 80 mmHg, it means that a person is not getting enough oxygen . A low PaO2 level can point to an underlying health condition, such as: emphysema. chronic obstructive pulmonary disease, or COPD.
What does PO2 mean in medical terms?
Values of partial pressure of oxygen (PO2) and of carbon dioxide (PCO2) were measured by means of blood gas electrodes.
Why is paco2 low?
The most common cause of decreased PCO2 is an absolute increase in ventilation. Decreased CO2 production without increased ventilation, such as during anesthesia, can also cause respiratory alkalosis. Decreased partial pressure of carbon dioxide will decrease acidity.
What is the PO2 in systemic arteries?
Systemic arterial pO2 averaged 71.1 { 11.0 mm Hg while arterial pCO2 and pH averaged 41.5 { 7.9 mm Hg and 7.38 { 0.05, respectively. Venous pO2 averaged 26.3 { 2.0 mm Hg and systemic arterial hematocrit was 45 { 1%.
What is the partial pressure of co2 in systemic arteries?
The partial pressure of carbon dioxide in systemic venous blood is normally 40 mmHg.
What is the value of PO2 in alveoli and tissues respectively?
159mm Hg, 40mm Hg.
What happens when partial pressure of carbon dioxide is increased?
When CO2 is elevated, it creates an acidic environment. In people with COPD who have serious breathing problems, the increased CO2 level can result in what is called respiratory acidosis.
How does partial pressure relate to gas exchange?
The greater the partial pressure of a gas, the more of that gas will dissolve in a liquid, as the gas moves toward equilibrium. Gas molecules move down a pressure gradient; in other words, gas moves from a region of high pressure to a region of low pressure.
What is external gas exchange?
External Respiration. External respiration is the formal term for gas exchange. It describes both the bulk flow of air into and out of the lungs and the transfer of oxygen and carbon dioxide into the bloodstream through diffusion.
What is the difference between PCO2 and TCO2?
PCO2 along with pH is used to assess acid-base balance. … TCO2 (total carbon dioxide) is either measured on plasma by automated chemistry analyzers or is cal cu lat ed from pH and PCO2 measured on whole blood gas analyzers.
What causes high co2 in blood?
Hypercapnia, or hypercarbia, is a condition that arises from having too much carbon dioxide in the blood. It is often caused by hypoventilation or disordered breathing where not enough oxygen enters the lungs and not enough carbon dioxide is emitted.
How do you find PaCO2?
- PaCO2 = 1.5 x HCO3 + 8 (+/- 2)
- PaCO2Delta = 1.2 x BicarbDelta.
- PaCO2 will not typically drop below 10 mmHg in respiratory compensation.
Where is the PCO2 the highest quizlet?
e) The Pco2 is lower at first in the capillaries than in the alveoli, and then it is higher in the alveoli than in the capillaries.
How co2 and O2 are transported in the blood?
Oxygen is carried both physically dissolved in the blood and chemically combined to hemoglobin. Carbon dioxide is carried physically dissolved in the blood, chemically combined to blood proteins as carbamino compounds, and as bicarbonate.





