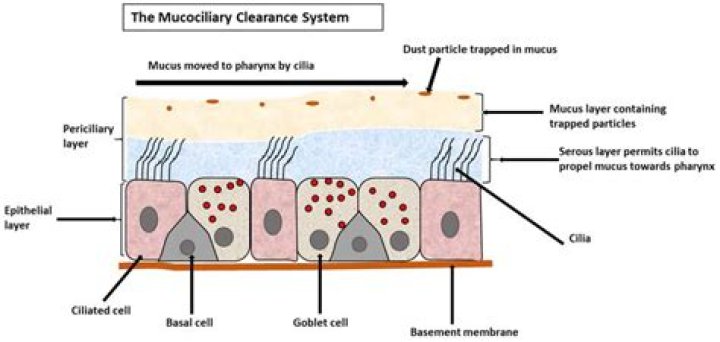
What is mucociliary blanket
 John Peck
John Peck This “mucociliary blanket” serves to filter our air of tiny particles which can contain infection and other irritants which are then digested by acid in our stomach. The mucus contains defensive proteins that help protect us from invasion by organisms.
What makes up the mucociliary blanket?
This term refers to the self-cleaning lining of the nose and sinuses which supports microscopically small hair-like filaments, called cilia, that rhythmically beat mucous through narrow sinus passageways towards the back of the nose and into the throat.
What is mucociliary system?
Mucociliary transport system. The mucociliary transport system provides the means for drainage of secretory products and particulate matter out of the sinuses. It is dependent on proper ciliary function and mucus viscosity.
Where is mucociliary blanket located?
The mucociliary blanket of the nasal cavity, trachea, and bronchi also plays an important role in preventing injury from toxic gases.Why is the mucociliary apparatus important?
Mucociliary clearance is an important primary innate defense mechanism that protects the lungs from deleterious effects of inhaled pollutants, allergens, and pathogens. Mucociliary dysfunction is a common feature of chronic airway diseases in humans.
What does clear jelly snot mean?
The consistency of your mucus is a sign from your body about what’s going on inside you. Mucus that’s runny and clear can mean that you have excess drainage coming from your nose. Mucus that’s green-tinged or yellow can mean that your sinuses have been exposed to an irritant, often an infection.
How does the mucociliary escalator clear your lungs from inhaled dust pollution?
The mucociliary escalator is inside of the conducting airways and is made up of mucus and cilia, which moves the mucus up and out of the lungs where it can be expelled by coughing or swallowing (Figures 1, 2) [5].
What does the mucous blanket cover?
A layer of protective mucus, called a mucus blanket, covers a large portion of the membrane lining the bronchial tree. … Microscopic, hair-like cilia move the cleansing mucus up to the pharynx—part of the throat between the mouth and esophagus—from the lower part of the bronchial tree.What in the human trachea produces mucus?
In the airways – the trachea, bronchi, and bronchioles, the lining of mucus is produced by specialized airway epithelial cells called goblet cells, and submucosal glands.
What increases mucociliary drainage?The rate of mucociliary clearance increases with greater hydration,2,73 and the rate of ciliary beating can be increased by purinergic, adrenergic, cholinergic, and adenosine-receptor agonists,60,73 as well as irritant chemicals. A second mechanism for the expulsion of mucus from the airways is cough clearance.
Article first time published onWhat is the purpose of surfactant in the lungs?
Pulmonary surfactant is essential for life as it lines the alveoli to lower surface tension, thereby preventing atelectasis during breathing. Surfactant is enriched with a relatively unique phospholipid, termed dipalmitoylphosphatidylcholine, and four surfactant-associated proteins, SP-A, SP-B, SP-C, and SP-D.
Can the lungs clean themselves?
Lungs are self-cleaning organs that will begin to heal themselves once they are no longer exposed to pollutants. The best way to ensure your lungs are healthy is by avoiding harmful toxins like cigarette smoke and air pollution, as well as getting regular exercise and eating well.
How does smoking affect mucociliary clearance?
The impairment in mucociliary clearance in individuals chronically exposed to cigarette smoke is associated with epithelial remodelling leading to structural abnormalities in the cilia, goblet cell metaplasia and mucous cell hypertrophy, resulting in increased mucus production [38,39].
What is blood gas barrier?
The blood–air barrier or air–blood barrier, (alveolar–capillary barrier or membrane) exists in the gas exchanging region of the lungs. It exists to prevent air bubbles from forming in the blood, and from blood entering the alveoli.
How can I increase my mucociliary clearance?
Heated, high-flow, humidified air or oxygen may improve mucus clearance by hydrating the mucus in the airways and may also help to increase airway patency. A similar intervention was shown to improve mucus clearance in subjects with bronchiectasis.
What causes impaired airway clearance?
Ineffective airway clearance can be an acute (e.g., postoperative recovery) or chronic (e.g., CVA or spinal cord injury) problem. High-risk for ineffective airway clearance are the aged individuals who have an increased incidence of emphysema and a higher prevalence of chronic cough or sputum production.
What will happen if the air sacs are damaged?
In emphysema, the inner walls of the lungs’ air sacs (alveoli) are damaged, causing them to eventually rupture. This creates one larger air space instead of many small ones and reduces the surface area available for gas exchange. Emphysema is a lung condition that causes shortness of breath.
Why are my boogers black?
Black mucus can materialize after inhaling dirt or dust; or after smoking cigarettes or marijuana. But it can also signal a serious fungal infection, especially if you have a compromised immune system. If your mucus is black for no obvious reason, you should see a doctor.
What color snot is bad?
Red or pink phlegm can be a more serious warning sign. Red or pink indicates that there is bleeding in the respiratory tract or lungs. Heavy coughing can cause bleeding by breaking the blood vessels in the lungs, leading to red phlegm. However, more serious conditions can also cause red or pink phlegm.
What's it mean when you cough up green phlegm?
If you see green or yellow phlegm, it’s usually a sign that your body is fighting an infection. The color comes from white blood cells. At first, you may notice yellow phlegm that then progresses into green phlegm. The change occurs with the severity and length of the potential sickness.
How do mucins prevent infection?
Mucins have direct and indirect roles in defense from infection distinct from their ability to form a physical barrier and act as adhesion decoys. Not only do mucin oligosaccharides bind microbes, but also, in some cases, they either have direct antimicrobial activity or carry other antimicrobial molecules.
How do I drain mucus from my lungs?
You lie down in different positions to help drain mucus from your lungs. Chest percussion. You lightly tap your chest and back. The tapping loosens the mucus in your lungs.
Does mucus fight virus?
Mucus is our body’s equivalent to fly paper, it lines the nose trapping the dirt and germs stopping them from damaging the lungs. But it does better than just sticking to them – mucus is loaded with protective proteins that kill and disable germs, like bacteria and viruses.
Does the mucus blanket cover the epiglottis?
The Mucous blanket covers all of the structures of the respiratory system except the Epiglottis.
What is the Sol layer?
The bronchial wall epithelium is lined with microscopic, hair-like structures called cilia which are surrounded by a thin film of fluid, called the sol layer.
Where is the paranasal sinus?
The paranasal sinuses are air-filled spaces located within the bones of the skull and facial bones.
How do you promote expectoration?
Breathing techniques, such as active cycle of breathing, body positioning and manual techniques, including percussion, shaking and vibrations, can also be used to loosen secretions and thus facilitate expectoration.
How can I stop phlegm at night?
- Use an extra pillow. …
- Avoid eating right before bed if you’re prone to acid reflux. …
- Take a steamy shower before bed. …
- Use a humidifier. …
- Take an expectorant. …
- Stay well-hydrated. …
- If your symptoms do not improve over a week or worsen suddenly, please consult a physician.
Which surfactant is important for lungs?
Pulmonary surfactant is essential for life as it lines the alveoli to lower surface tension, thereby preventing atelectasis during breathing. Surfactant is enriched with a relatively unique phospholipid, termed dipalmitoylphosphatidylcholine, and four surfactant-associated proteins, SP-A, SP-B, SP-C, and SP-D.
What is the inflammation of the lining that covers the lungs?
Pleurisy occurs when the pleura — a membrane consisting of a layer of tissue that lines the chest cavity and a layer of tissue that surrounds the lungs — becomes inflamed, causing chest pain.
Can you give surfactant to adults?
Administration of exogenous pulmonary surfactant is an adjunctive therapy that may help adult patients with ARDS. Pulmonary surfactant is produced by type II alveolar cells and is composed of two major fractions: phospholipids (90%) and surfactant-specific proteins (10%).





