What is Aki in medical terms
 Christopher Martinez
Christopher Martinez Acute kidney injury (AKI) is where your kidneys suddenly stop working properly. It can range from minor loss of kidney function to complete kidney failure. AKI normally happens as a complication of another serious illness. It’s not the result of a physical blow to the kidneys, as the name might suggest.
What are the 3 stages of AKI?
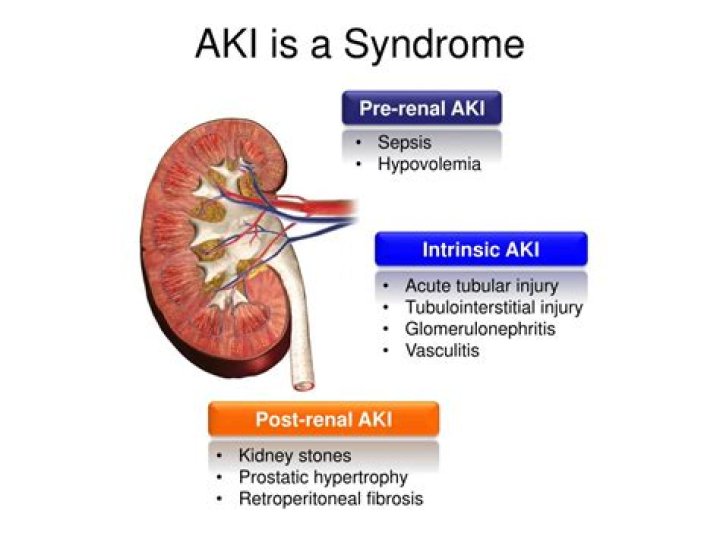
AKI occurs in three types—prerenal, intrinsic, and postrenal.
How long can you live with AKI?
In a long-term follow-up study of 350 patients from the randomized RENAL trial who survived AKI in the intensive care unit, researchers found that the overall mortality rate was 62% at a median of 42.4 months after randomization.
What is AKI warning stage?
in Primary Care From April of this year primary care will start receiving Acute Kidney Injury (AKI) warning stage test results which are generated when a significant change in creatinine concentration is measured.What is the most common cause of death in AKI?
Infections commonly complicate the course of AKI and have been reported to occur in as many as 33% of patients with AKI. The most common sites of infection are the pulmonary and urinary tracts. Infections are the leading cause of morbidity and death in patients with AKI.
Is AKI life threatening?
It is important that AKI is found as soon as possible because it can lead to chronic kidney disease, or even kidney failure. It may also lead to heart disease or death.
How long does it take to recover from AKI?
In some cases AKI may resolve in a couple of days with fluid and antibiotics. In other cases the illness affecting the kidneys and the rest of the body may be so severe that recovery takes two or three weeks or even longer.
How do hospitals treat AKI?
If your acute kidney failure is caused by a lack of fluids in your blood, your doctor may recommend intravenous (IV) fluids. In other cases, acute kidney failure may cause you to have too much fluid, leading to swelling in your arms and legs.What are the complications of AKI?
- high levels of potassium in the blood – in severe cases, this can lead to muscle weakness, paralysis and heart rhythm problems.
- fluid in the lungs (pulmonary oedema)
- acidic blood (metabolic acidosis) – which can cause nausea, vomiting, drowsiness and breathlessness.
- Water retention/swelling of legs and feet.
- Loss of appetite, nausea, and vomiting.
- Confusion.
- Shortness of breath.
- Insomnia and sleep issues.
- Itchiness, cramps, and muscle twitches.
- Passing very little or no urine.
- Drowsiness and fatigue.
Can UTI cause AKI?
Our study found that patients with upper UTI had higher risk of AKI than those with lower UTI (OR 2.63, 95% CI 1.53–4.56, P = 0.001). Early institution of appropriate antibiotic therapy for patients with upper UTI, especially those with septic shock, is important to prevent the development of AKI.
What happens when kidneys start to shut down?
Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes may accumulate, and your blood’s chemical makeup may get out of balance.
What is AKI stage1?
AKI stage 1 is a rise of ≥1.5x baseline level, which is known or presumed to have occurred within the. prior 7 days; or of >26 micromol/L within 48h, or a urine output <0.5mL/kg/h for 6-12h.
Is AKI reversible?
AKI is sometimes called acute kidney failure or acute renal failure. It is very serious and requires immediate treatment. Unlike kidney failure that results from kidney damage that gets worse slowly, AKI is often reversible if it is found and treated quickly.
What color is urine when your kidneys are failing?
Brown, red, or purple urine Kidneys make urine, so when the kidneys are failing, the urine may change. How? You may urinate less often, or in smaller amounts than usual, with dark-colored urine. Your urine may contain blood.
What are the chances of surviving acute kidney failure?
The survival rate is nearly 0% among patients with AKI who have an Acute Physiology and Chronic Health Evaluation II (APACHE II) score higher than 40. In patients with APACHE II scores of 10-19, the survival rate is 40%.
What drugs should be stopped in Aki?
All drugs which block renal excretion of potassium (trimethoprin and potassium sparing diuretics (spironolactone, amiloride) should be stopped. In addition, both beta-blockers and digoxin can inhibit the sodium / potassium ATPase pumps which move potassium inside cells.
Can kidneys repair themselves after acute kidney failure?
Acute kidney failure requires immediate treatment. The good news is that acute kidney failure can often be reversed. The kidneys usually start working again within several weeks to months after the underlying cause has been treated. Dialysis is needed until then.
Can you have CKD and Aki?
Acute kidney injury (AKI) is a common disorder, with a population incidence of about 2,000 per million population (pmp). Patients with chronic kidney disease (CKD), as evidenced by a low eGFR or presence of proteinuria, are at higher risk for developing AKI, a condition known as acute on chronic renal failure (ACRF).
Is drinking a lot of water good for your kidneys?
Water helps the kidneys remove wastes from your blood in the form of urine. Water also helps keep your blood vessels open so that blood can travel freely to your kidneys, and deliver essential nutrients to them.
How do you know if Covid is affecting your kidneys?
Signs of kidney problems in patients with COVID-19 include high levels of protein in the urine and abnormal blood work. The kidney damage is, in some cases, severe enough to require dialysis.
What foods prevent kidney failure?
A kidney-friendly diet should limit sodium, cholesterol, and fat and instead focus on fruits, vegetables, whole grains, low-fat dairy, and lean meats (seafood, poultry, eggs, legumes, nuts, seeds, and soy products), says Maruschak.
What tests can be done to determine the cause of Aki?
Evaluation should determine the presence and type of AKI and seek a cause. Blood tests generally include complete blood count (CBC), BUN, creatinine, and electrolytes (including calcium and phosphate). Urine tests include sodium, urea, protein, and creatinine concentration; and microscopic analysis of sediment.
Is dying of kidney failure painful?
Is death from kidney failure painful? Not usually. If you do feel any discomfort, pain medication may be prescribed for you. Without treatment for kidney failure, toxins, and fluid will build up in your body, making you feel increasingly tired, nauseous and itchy.
How do you know when death is hours away?
Hours Before Death Symptoms In the final hours of life, your loved one’s body will begin to shut down. Their circulatory and pulmonary systems will slowly begin to fail. This may lead to falling body temperatures, but may also cause sudden outbursts.
What organs shut down first when dying?
The brain is the first organ to begin to break down, and other organs follow suit. Living bacteria in the body, particularly in the bowels, play a major role in this decomposition process, or putrefaction.
Is hydronephrosis an Aki?
If acute kidney injury is caused by a blockage (an obstruction), the backup of urine within the kidneys causes the drainage system to stretch (a condition called hydronephrosis—see figure Hydronephrosis—A Distended Kidney.
Where do you itch with kidney disease?
It can come and go or it may be continuous. It may affect your whole body or be limited to a specific area – usually your back or arms. Itching tends to affects both sides of the body at the same time and may feel internal, like a crawling feeling just below the skin.
Does kidney disease affect walking?
The studies revealed a primary emphasis on gait speed measures within clinical tests, and a neglect of spatiotemporal gait variables. Most of the studies showed that CKD progression is associated with slowing of walking speed.
What is the major cause of kidney failure?
Diabetes and high blood pressure are the most common causes of chronic kidney disease (CKD).
What is baseline creatinine?
The investigators defined the baseline serum creatinine as the lowest, most recent, or the median value over the preadmission period. The team used a joint model that combined a linear mixed model for repeated inpatient serum creatinine relative to baseline value and a Cox proportional survival model.