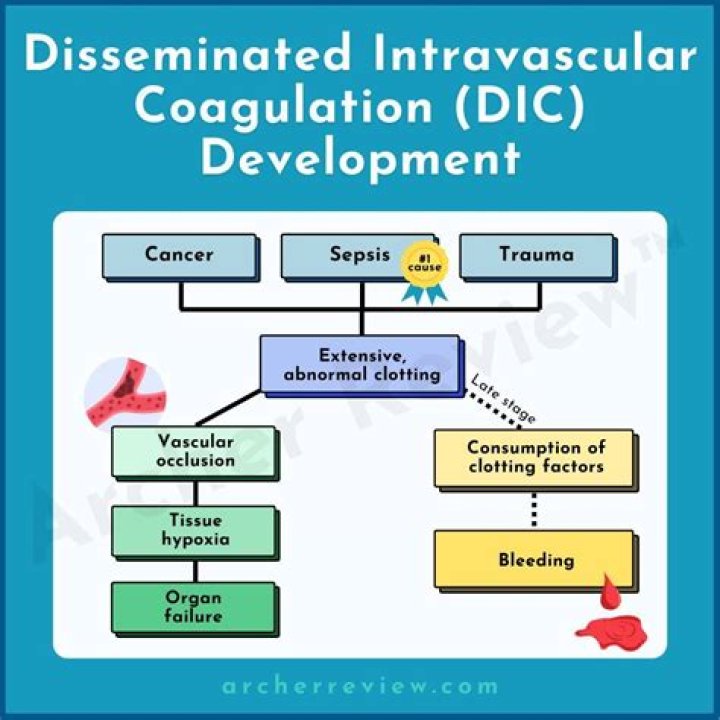
What causes disseminated intravascular coagulation
 Rachel Young
Rachel Young The underlying cause is usually due to inflammation, infection, or cancer. In some cases of DIC, small blood clots form in the blood vessels. Some of these clots can clog the vessels and cut off the normal blood supply to organs such as the liver, brain, or kidneys.
What bacteria causes disseminated intravascular coagulation?
DIC is classically associated with Gram negative bacterial infections but it can occur with a similar incidence in Gram positive sepsis. Moreover, systemic infections with other micro-organisms, such as viruses, Rickettsiae and even parasites (e.g. Plasmodium falciparum) may also result in DIC.
Why is disseminated intravascular coagulation life threatening?
Disseminated intravascular coagulation (DIC) is a rare, life-threatening condition. In the early stages of the condition, DIC causes your blood to clot excessively. As a result, blood clots may reduce blood flow and block blood from reaching bodily organs.
Who is at risk for disseminated intravascular coagulation?
People who have one or more of the following conditions are most likely to develop DIC: Sepsis (an infection in the bloodstream) Surgery and trauma. Cancer.What virus causes DIC?
DIC is not frequently encountered in other viral infections [51, 52] but has been found in cases of rotavirus [53, 54], varicella, rubella, rubeola, and influenza infections [55–61].
What is a classic symptom of DIC?
DIC may develop quickly over hours or days, or more slowly. Signs and symptoms may include bleeding, bruising, low blood pressure, shortness of breath, or confusion. Complications can be life-threatening and include bleeding or multiple organ failure.
How can you prevent disseminated intravascular coagulation?
- Plasma transfusions to reduce bleeding. Plasma transfusion replace blood clotting factors affected by DIC.
- Transfusions of red blood cells and/or platelets.
- Anti-coagulant medication (blood thinners) to prevent blood clotting.
Does DIC cause thrombocytopenia?
Severe, rapid-onset DIC causes severe thrombocytopenia, prolonged prothrombin time and partial thromboplastin time, a rapidly declining plasma fibrinogen level, and a high plasma D-dimer level.Can you survive DIC?
The long-term outlook for people who have DIC depends on how much damage the clots may have caused to the body’s tissues. About half of those with DIC survive, but some may with live with organ dysfunction or the results of amputations.
How does trauma cause DIC?The resulting coagulopathy is characterized by nonsurgical bleeding from mucosal lesions, serosal surfaces, and wound and vascular access sites. DIC associated with traumatic injury results from multiple independent but interplaying mechanisms, involving tissue trauma, shock, and inflammation.
Article first time published onWhat is a supportive treatment for a client with disseminated intravascular coagulation?
The goal is to determine and treat the underlying cause of DIC. Supportive treatments may include: Plasma transfusions to replace blood clotting factors if a large amount of bleeding is occurring. Blood thinner medicine (heparin) to prevent blood clotting if a large amount of clotting is occurring.
How do you diagnose DIC?
To diagnose DIC, your doctor may recommend blood tests to look at your blood cells and the clotting process. For these tests, a small amount of blood is drawn from a blood vessel, usually in your arm.
Which clinical manifestations of disseminated intravascular coagulation are due to the depletion of clotting factors?
Acute DIC is a haemorrhagic disorder characterised by multiple bruises (ecchymoses), bleeding from mucosal sites (such as lips and genitals) and depletion of platelets and clotting factors in the blood. Purpura fulminans is a severe and rapidly fatal form of acute DIC.
What Gram negative bacteria causes DIC?
Overt/decompensated DICInfection • Gram-negative bacteria (endotoxins) • Gram-positive bacteria (mucopolysaccharides)Intravascular haemolysis • Haemolytic transfusion reaction • Haemolysis • Massive transfusion
How does sepsis cause DIC?
Sepsis-induced DIC. During sepsis, inflammation diffusely activates the coagulation system, consuming multiple clotting factors and resulting in DIC [10, 11].
Which assessment finding would indicate that a client has developed disseminated intravascular coagulation?
Diagnosis of DIC involves a combination of laboratory tests and clinical evaluation. Laboratory findings suggestive of DIC include a low platelet count, elevated D-dimer concentration, decreased fibrinogen concentration, and prolongation of clotting times such as prothrombin time (PT).
What is the mortality rate of DIC?
Patients with DIC scores >or= 5 (overt DIC) had 50% mortality, compared to 20% for patients with DIC scores < 5. Overall, a one-point rise in DIC score was associated with an increased risk of mortality after adjusting for age, race, gender, hemodynamic instability, and PRISM III score [OR 1.35 (1.02, 1.78)].
What is the survival rate for DIC?
Mortality in ED patients with DIC Mortality rates range from 40 to 78% in hospitalized patients experiencing DIC 3,19. The presence of DIC in ED patients results in roughly comparable overall 30-day mortality rates (52%).
Is LDH elevated in DIC?
We recently reported that patients with hemophagocytic lymphohistiocytosis (HLH) who developed DIC and/or hepatobiliary dysfunction (HBD) have increased risk of death 4. LDH is elevated in patients with HLH, but the clinical significance of this laboratory value is unknown.
Is LDH high in DIC?
In the laboratory schistocytes are prominent in the blood smear and LDH levels usually more pronounced than in DIC, while most conventional coagulation markers are normal.
What suppresses fibrinolytic activity in the pathogenesis of disseminated intravascular coagulation DIC )?
However, this profibrinolytic response is almost immediately followed by suppression of fibrinolytic activity due to a sustained increase in plasma levels of PAI-1 ; these effects are mediated by TNF-2 and IL-1.
How does eclampsia cause DIC?
The process of DIC is initiated through the activation of tissue factor (TF), which is found in subendothelial cells, amniotic fluid, and placenta. DIC is seen in severe forms of preeclampsia with hemolysis, elevated liver enzymes, and low platelet count (HELLP) syndrome.
Can liver cause DIC?
Patients with hepatic failure may present with the entire spectrum of factor deficiencies and may even develop disseminated intravascular coagulation (DIC). Patients with liver cirrhosis have a wide spectrum of abnormalities.
How is coagulopathy treated?
The overall goal of coagulopathy treatment is to improve the blood’s ability to clot, but the specific treatment largely depends on the underlying cause. Therapy to improve the blood’s ability to clot may include replacing the missing clotting factors or increasing platelet levels through transfusion.
How would you treat a patient with intravascular coagulation?
Management of patients who present with acute promyelocytic leukemia and DIC consists of supportive treatment with platelet transfusion (aiming at a platelet count of >30-50 × 109/L), fresh frozen plasma, and fibrinogen concentrate (guided by the fibrinogen concentration in the patient’s plasma) and should be …
Do you agree that disseminated intravascular coagulation DIC leads to Hypocoagulation?
DIC is characterized by the systemic activation of coagulation, leading to widespread microvascular thrombosis, which compromises organ perfusion and can contribute to organ failure. The ongoing activation of coagulation may exhaust platelet and coagulation factors, resulting in a hypocoagulable state and bleeding.
Does disseminated intravascular coagulation lead to Hypercoagulation?
Disseminated intravascular coagulation can be defined is a widespread hypercoagulable state that can lead to both microvascular and macrovascular clotting and compromised blood flow, ultimately resulting in multiple organ dysfunction syndrome.
What is the most sensitive marker for DIC?
In a specialized setting, molecular markers for activation of coagulation or fibrin formation may be the most sensitive assays for DIC. A number of clinical studies show that the presence of soluble fibrin in plasma has a 90-100% sensitivity for DIC but, unfortunately, a relatively low specificity.
Why do you give heparin for DIC?
Heparin, as an anticoagulant, which, not only inhibits the activation of the coagulation system, but is also an anti-inflammatory and immunomodulatory agent, has been widely used during DIC treatment and in the prevention and treatment of thrombotic diseases.
Can DIC cause pulmonary embolism?
In conclusion, based on the present findings massive pulmonary embolism in combination with cardiopulmonary resuscitation can be associated with DIC.
How do endotoxins cause DIC?
Excessive activation of the coagulation system by endotoxin leads to life- threatening disseminated intravascular coagulation (DIC).