Degree: Bachelor of Science.
Considering this, how much do utilization review nurses make?
The national average salary for a Utilization Review Nurse is $72,114 in United States.
how do I become an utilization reviewer? Research the requirements to become a utilization nurse.
Career Requirements.
| Degree Level | Minimum of associate's degree is required (many employers prefer a bachelor's degree) |
| Experience | 2-5 years of experience as an RN; some experience in case management or utilization review |
In this regard, how do I become a Utilization Management Nurse?
A utilization review nurse ensures that the hospital implements the most appropriate care plans for its patients. Become a utilization review nurse by earning a Bachelor of Science in Nursing (BSN). Pass the NCLEX-RN (National Council Licensure Examination for RNs) exam to become a registered nurse in a hospital.
Why do you want to be a utilization review nurse?
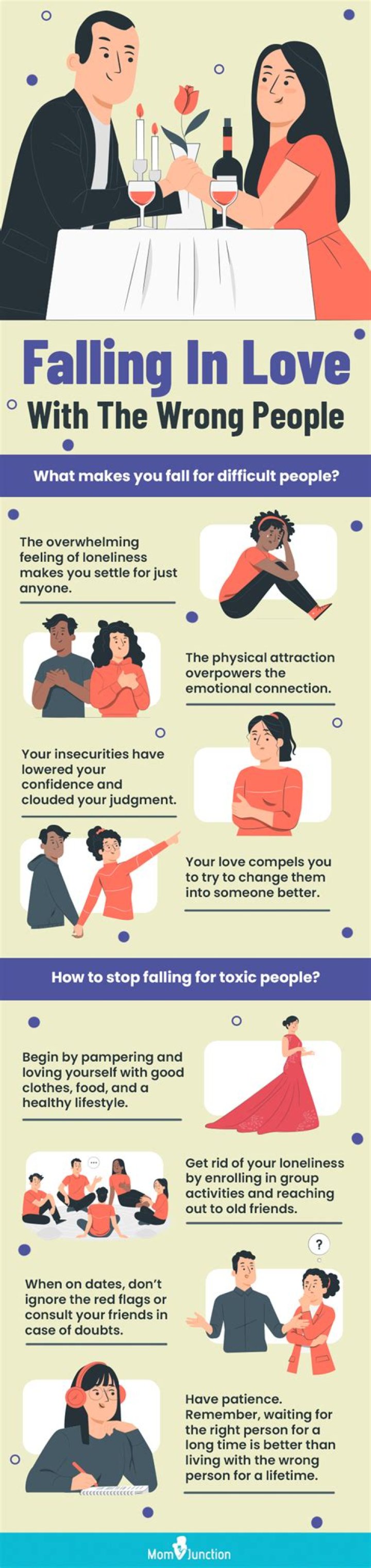
Utilization review (UR) nurses work behind the scenes to maximize the quality and cost efficiency of health care services. UR nurses also help insured persons to make informed decisions about their health care by educating them on the benefits and limitations of their Medicare, Medicaid or private health care coverage.
Related Question Answers
What is the difference between utilization review and case management?
The difference is that utilization management is a prospective process that occurs before and during the admission, procedure or treatment, while utilization review is retrospective.How much does a utilization reviewer make?
A mid-career Utilization Review Specialist with 5-9 years of experience earns an average total compensation of $19.98 based on 66 salaries. An experienced Utilization Review Specialist with 10-19 years of experience earns an average total compensation of $22.97 based on 60 salaries.How much do RN case managers make?
Salary Prospects The median salary for registered nurse case managers is $64,000. The lowest 10% earn $47,830 or below, and the top 10% earn $83,370 and above. The top 10% tend to be those with the highest levels of education, including doctorate degrees.How much do nurses make at insurance companies?
The annual median salary for nurses in insurance is $80,090.What are the responsibilities of a utilization review nurse?
Summary: Utilization Review Nurses are Registered Nurses who review patient files or information and check if proper care is being rendered. With Utilization Review Nurses that work in insurance companies, their job is to review medical claims and determine whether they are paid or not. They serve as consultants.How much does a clinical review nurse make?
The national average Clinical Review Nurse salary is $75,429. Filter by location to see Clinical Review Nurse salaries in your area. Salary estimates are based on 1,119 salaries submitted anonymously to Glassdoor by Clinical Review Nurse employees.How much does a prior authorization nurse make?
The national average salary for a Prior Authorization RN is $65,870 in United States. Filter by location to see Prior Authorization RN salaries in your area.How much do telephonic nurses make?
A Telephonic Nurse earns an average wage of $28.81 per hour. Is Telephonic Nurse your job title? Get a personalized salary report!What is InterQual and Milliman?
Guidelines like InterQual® and Milliman (now “MCG”), are often recommended and used as the standards to apply for admission decision making. They are based, at least in part, on information gleaned from the medical literature and have been clinically validated by their successful application for several decades now.How much does a utilization manager make?
The average salary for a Utilization Manager is $76,138 per year in the United States.What is a certified managed care nurse?
Managed Care Nurses serve as the liaison between patients, doctors, healthcare providers and Insurance companies. In contrast to direct patient care at the bedside, their role is to advocate for all patients enrolled in the healthcare delivery system. The overall goal of a Managed Care Nurse is patient advocacy.What is InterQual level of care criteria?
InterQual® Level of Care Criteria. Assess the safest and most efficient care level based on severity of illness, comorbidities, complications, and the intensity of services being delivered.How Much Does a Medical Review Nurse make?
The average pay for a Medical Review Nurse is $36.00 per hour. The average pay for a Medical Review Nurse is $62,763 per year. Is Medical Review Nurse your job title?What does a utilization manager do?
According to URAC, an accreditor of health care organizations, utilization management is "the evaluation of the medical necessity, appropriateness, and efficiency of the use of health care services, procedures, and facilities under the provisions of the applicable health benefits plan, sometimes called 'utilizationWhat are the steps of the utilization review process?
There are three activities within the utilization review process: prospective, concurrent and retrospective. Prospective review includes the review of medical necessity for the performance of services or scheduled procedures before admission.Why do you want to work in utilization management?
The primary goal of someone working in utilization management is to help manage the care the health plan member (meaning the patient) gets through their benefits, so that patient can return to his or her normal daily tasks.What is a nurse reviewer?
Job Description for Registered Nurse (RN), Utilization Review (UR) The primary responsibility of the utilization review nurse is to review medical records and prepare clinical appeals (when appropriate) on medical necessity, level of care, length of stay, and authorization denials for hospitalized patients.What does a hedis review nurse do?
What do HEDIS nurses do? They collect and review data from patient charts and other medical records from hospitals, doctors' offices and various health care providers to measure and help improve quality.What is utilization review in hospitals?
Utilization review is the process of making sure health care services are being used appropriately. The goal of utilization review is to make sure patients get the care they need, that it's administered via proven methods, provided by an appropriate health care provider, and delivered in an appropriate setting. 
 William Burgess
William Burgess